Disease interception – What does it mean and why is it important? (Guest blog)
21.09.17
As we speak, many people are scrutinising developing drugs that work at earlier time points in the disease process. This concept is called disease interception.
There are differing opinions as to what disease interception is and so it is important to understand and agree what is meant by the term. Generally, the definition of interception relies on three key factors.
1. Ideally the individual should have no symptoms of disease. If they do have symptoms it may well be too late for disease interception.
2. You should be able to detect a medical marker that can be seen before the patient develops disease symptoms.
3. You should then be able to treat medically and stop the patient from having disease symptoms based on the detection of this marker.
But what would this look like in reality?
An example would be if you detected high cholesterol in someone following a blood test. There are no symptoms as you cannot see or feel high cholesterol. However, if left untreated, this would be a contributor to future cardiovascular disease, leading possibly to heart attack or stroke. If you then gave this person a drug that reduces their cholesterol, this treatment would be called disease interception. In this example the patient has no symptoms, cholesterol is the medical marker and the treatment is intercepting the cardiovascular disease before it can develop. This meets the three key factors mentioned earlier.
One area of common confusion is the difference between disease prevention and interception. It may be useful to refer to the three key factors. If a person’s disease is prevented, they would have no symptoms and so would meet one of the key factors. But there are no medical markers or medical treatments and, as such, prevention does not meet these factors.
To put this in context with our example, disease prevention in heart disease may be to stop smoking, a change of diet or the introduction of an exercise regime. This would be classed as prevention rather than interception because no medical marker is being measured and no medical treatment is being given. Another common example of prevention would be vaccines, as they too do not rely on medical markers.
In the prevention arena, there is often regulatory guidance, a tried and tested pathway to develop drugs and an understanding of the needs of key stakeholders (e.g. regulators, Health Technology Assessments bodies, the medical community etc.)
The situation becomes less clear when disease interception is considered, where precedence is both inconsistent and limited to a few specific conditions (e.g. the development of statins to treat high cholesterol). However, in other disease areas the situation is less clear as it is in dementia, cancer treatment or diabetes.
So far we have identified several key areas of challenge, including those shown in the diagram below:
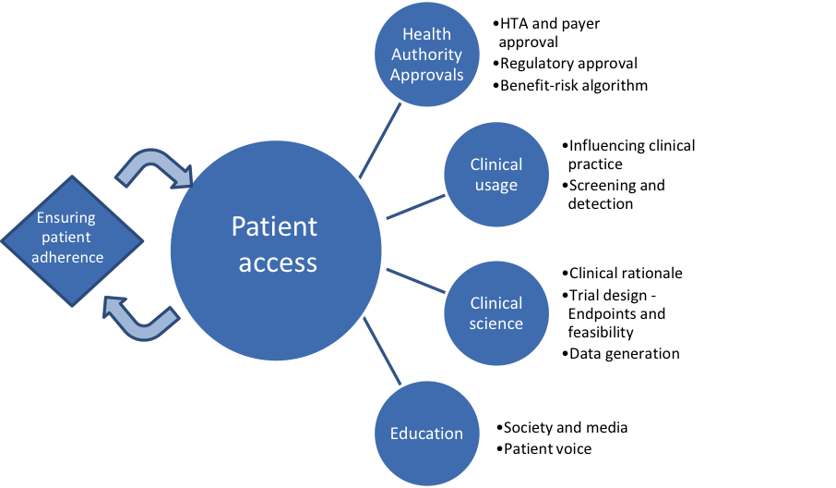
In conclusion, there is both a clear need and responsibility to make sure that all the key stakeholders involved in the provision of medicines to individuals are prepared for the challenges and opportunities that disease interception brings. We all need to ensure that there are as few disincentives as possible to developing, approving and delivering disease interception drugs to society. With this in mind, we are working hard to support the ongoing work in disease interception and to raise awareness of the challenges of developing drugs in this setting.
